The new combination of active substances they identified will have to undergo clinical trials before they can be used to treat patients. The researchers published their results in the prestigious scientific journal Science Translational Medicine.
Lack of protein DJ-1 makes you sick
A protein called DJ-1 plays a crucial role in keeping nerve cells functioning. If the body is unable to produce ample amounts of DJ-1, important nerve cells die. The result is the onset of neuro-degenerative diseases such as Parkinson’s. The production of important proteins like DJ-1 can be disrupted or halted permanently if the genetic blueprints or the production processes they encode are defective.
Prof. Rejko Krüger’s research team has identified for the first time the importance of an error in the production process of DJ-1 in the development of a certain form of Parkinson’s disease. “In the patients, an essential tool for the assembly of the protein DJ-1 fails to dock properly,” Krüger explains. “As a result of this defect, the protein doesn’t get built at all.” The research result offers an entirely new point of attack for treating this malfunction of protein synthesis with drugs. “In this case, this insight fundamentally changes our view of the causes of the disease and presents entirely new possibilities for treatment,” says Dr Ibrahim Boussaad, first author of the scientific paper. “We could only gain this new understanding thanks to the skin cells from the patients,” Boussaad emphasises.
Cell donation enables progress
Thanks to the donation of skin cells by patients and healthy volunteers, the researchers in Luxembourg were able to reprogram these cells to grow into nerve cells in vitro. These nerve cells are very similar to the neurons in the donor’s brain and can be used for analyses and tests in the laboratory. Because it is not possible to take neurons directly from the brain of patients, for health and ethical reasons, reprogramming is the only way to examine the clinical features of the patient’s neurons in vitro.
“Each sample donated by a patient or a control individual is important,” highlights Prof. Krüger. “There are many genetic mutations that can each have a different impact. To identify the diverse mechanisms involved in Parkinson’s disease, it is crucial to collect as many samples as possible and study cells derived from the respective mutation carriers. And what we find in one patient might help us not only to understand what is happening in other cases, but also to identify a group of patients that may profit from the same new treatment.” 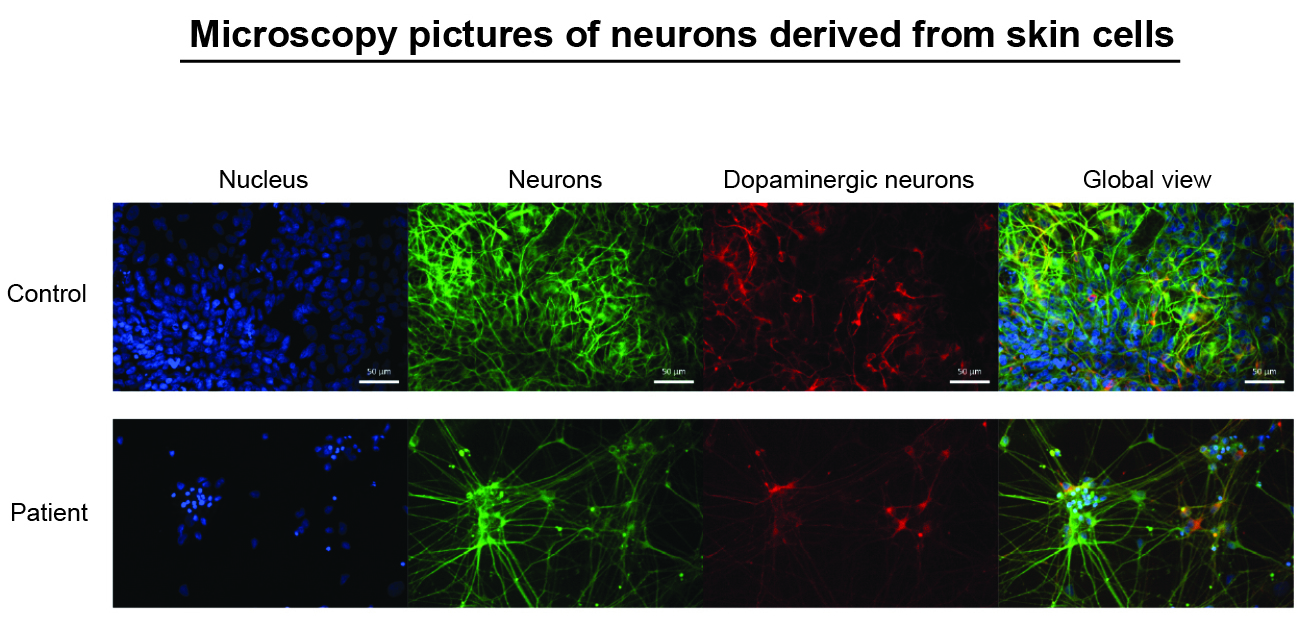
Luxembourg’s interdisciplinarity is a key to this success
In this recent study, using the patient-derived neurons, Prof. Krüger’s team was able to explain the cause of the genetic form of Parkinson’s disease in which the PARK7 gene is mutated. Then, precise bioinformatics tools developed at the Luxembourg Centre for Systems Biomedicine allowed the researchers to immediately carry out an automated search for potential active substances for drug treatment. Two active compounds – called phenylbutyric acid and RECTAS – were identified. Administered in combination, these two substances allow the cells in the test tube to effectively reactivate the production of the important protein DJ-1.
“Only by combining numerous disciplines, from medical practice, to laboratory research, to computer science, could we understand the cause and at the same time identify active substances for a potential treatment,” Prof. Rejko Krüger explains. He adds, “This kind of scientific progress ‘Made in Luxembourg’ is possible because all the necessary disciplines have been unified in Luxembourg for several years now.” The team of scientists especially expresses its gratitude to the people who are participating in the Luxembourg Parkinson’s Study and who have made this research possible in the first place.
To know more, read the press release and full scientific article.



